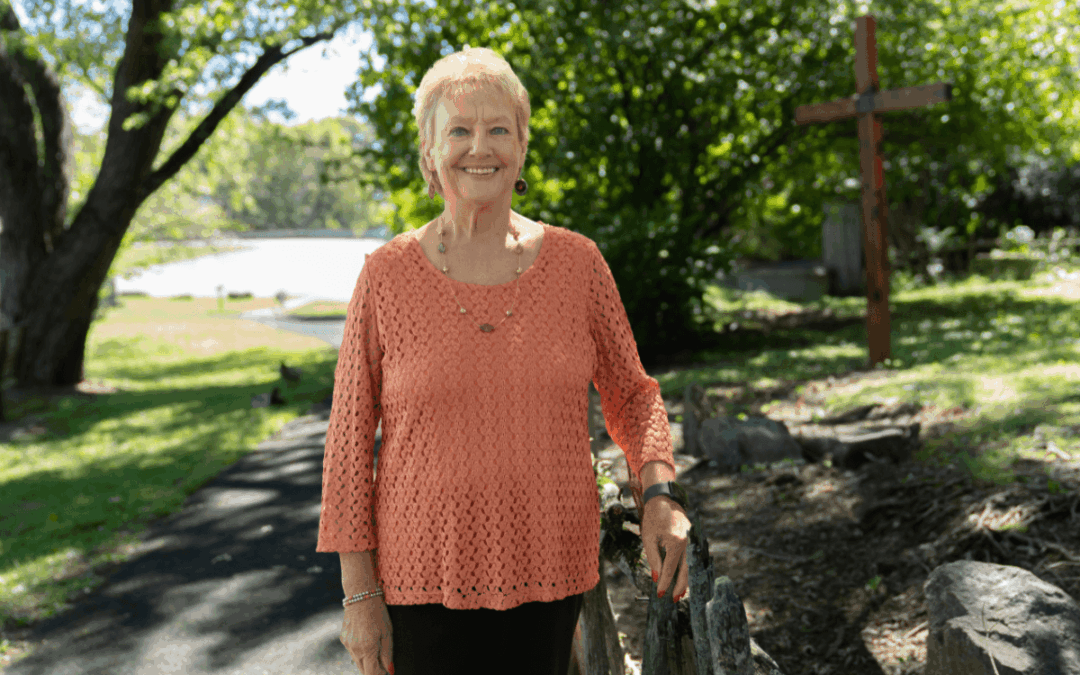IT WAS a time when the world and healthcare resembled a sci-fi horror movie more than the world we’d known. At least our world before the pandemic was larger than theirs. The world of patients confined to skilled care centers is small, occupied by those who can no longer care for themselves and those who watch over them. On a good day, friends, family, and others from the community come and go and break up the day’s monotony. Time is measured less by the hour and minute and more by the facility’s routines.
But COVID shut down their world, too.
“We were all they had. It was a really tough time, seeing people visit their family through the window,” said Gloria Armstrong. “I can’t imagine what the nurses in these big hospitals went through. You were scared you would get sick or take something home to your family. Quite a few of us got sick, but we were blessed. We didn’t lose the staff, but we did lose a lot of our sweet little patients.”
The Donalson Care Center treatment nurse was both a caregiver and a family member during this time. And not just to residents.

“My dad was a patient here then, and I could see him when I worked, but I didn’t get to see him when I was off. I was blessed that I was working here,” Armstrong said.
She entered healthcare as a certified nursing assistant (CNA) three months after high school graduation, using the skills she learned in her health occupations class. About five years later, she became a licensed practical nurse and has been in the system for more than 42 years. Armstrong has worked at Lincoln Care Center and Donalson Care Center. She has seen the evolution of healthcare in her time.
“We have a lot more modern conveniences [now]. [In the past], we had old metal bedpans and glass thermometers, and we had to clean [them] all. Everything’s just different now,” Armstrong said. “We never had computers [before]. [Now], we have different medicines and things like lifts to help with the patients. There’s been a lot of changes. I won’t say it’s bad, but I’m not a big fan of change.”
Another thing that’s changed is her ability to relate to the families of her patients.
“My husband was pretty sick about 16 years ago, and I’m not saying I didn’t care about people then, but things really shifted when I saw it from the other side. I try to treat people like I wanted him to be treated,” she said. “As you age, you realize you might be here someday. You have to put yourself in the patient’s shoes, and you have to put yourself in the families’ shoes.”

In some instances, though, the staff is the only family a resident may have.
Armstrong said, “For most people, this is their last home, and we’ve just got to make it as comfortable for them as possible. That’s our goal. I see many of these CNAs — they don’t make a lot of money — spending their money bringing body wash in here so the patients will have something other than the institutional wash, picking them up [something from] Sonic —doing stuff like that. I think that’s neat. And then some of them here don’t have any family; their family is gone, so the girls are good to pick up the slack and do some special things.”
Armstrong is a treatment nurse specializing in wound care. In a long-term facility, we often associate wounds with bed sores. The source of wounds needing care varies greatly.
She said, “It’s related to a lot of things like their condition and whether or not they’re eating. They may get wounds on their heels if they’ve had to be on the operating table. Mostly, it goes along with diabetes; it’s hard to heal skin with that [disease]. And when they’re getting sicker, it’s when it develops. It happens when they’re not eating because you have to have protein. I tell families your skin is an organ just like your heart, and it wears out. It gets old, just like the rest of your body. Many people think it’s from neglect, but most of the time, it’s due to the patient’s overall condition. They have a lot of comorbidities.”

The hours are long, and the work is demanding.
“It’s very hard physical work, and it’s hard emotional work. Your family suffers, and you’ve got to work a lot of holidays and long hours. With 12-hour shifts, you miss a lot, and your family has to sacrifice,” said Armstrong. “My husband, Doug, has been a godsend. He gets a little frustrated, but, for the most part, over the years, he’s gone along with it.” The years have been many, and the rewards have been great.
She said, “I just like to see their smiles. I have a little lady who is 95, and she calls out to me when I go by. The other day, she said, ‘It just makes me so happy to see you on the days you’re here.’ And I’ve met a lot of families — people that stay in contact with me even after their loved one has died.”
What she has seen reminds her daily of something we often forget.
“Be thankful for your health and your family because it can change in an instant. Treat others as you want to be treated, and love on the people in your life. Your health is a one-time thing, and once it’s gone, it’s gone,” said Armstrong. GN